|
Chapter 3 Health Protection |
| 1. Maternal and Child Health |
|
Japan's infant mortality used to be as high as 150-160 per thousand births until early 20th century but declined sharply to below 10 in 1975. Japan's current figure of 3.2 (2000) is one of the lowest even among developed countries. This may well be regarded as a triumph of Japan's post war MCH policy. According to the MCH Act, pregnant mothers are required to report to the municipal governments and the MCH notebook will be issued. This entitles her to public funded free health guidance and preventive medical activities as well as a health record for the child through the course of pregnancy and after birth. Health guidance and consultation by public health nurses may continue after birth especially when the new born babies are weighed 2500mg or less, in which case parents are required to report to the local public health centers to prompt them for quick action. All newborn babies are entitled for public funded mass screening to detect congenital metabolic diseases such as phenylketonuria, and for the babies born to HB positive mothers, immunoglobulin and vaccination will be provided as part of health insurance benefit. In 1994, nearly 2,500 newborns received immunoglobulin and vaccination for HB out of 1.127 million newborns. For very low birth weight babies who require intensive care after birth, health insurance coverage starts on the first day of their births as dependent family status of their parent's health insurance. The usually required 20-30% copayment will be waived by public funding for the babies whose birth weight below 2000g. All babies are entitled to free well-baby check ups twice at the age of 1.5 years and 3 years, all of which are provided by municipal governments. |
| 2. Elderly Health |
|
(1) The Elderly Health System (EHS) In response to population aging, the Elderly Welfare Act was implemented in 1963. It was later revised to subsidize the copayment of health insurance to guarantee easy access to health care starting in 1973. However the elimination of copayment drastically inflated the health care cost for the elderly and financially distressed the National Health Insurance system run by municipal governments because of uneven distribution of elderly enrollment among different insurance systems. There was a strong call for total unification of fragmented health insurance system for better risk sharing of the elderly health care cost, but such solutions were not likely to come by because of strong opposition from industry side. As an alternative, the Elderly Health Act was implemented to introduce a financial redistribution mechanism among different health insurance systems to equalize the disparity of elderly enrollment, which took effect in 1983. (2) Health Care component of the EHS After the implementation of the EHS, health care cost for the elderly 70 years old or over was financed in a somewhat different manner than ordinary population. While the elderly population are also enrolled to health insurance system and pay the same premium with the younger population, their health care cost are paid by municipal governments where the elderly resides. All the health insurers contribute to a newly created financial pool managed by a public corporation and the amount of contribution of individual insurers are calculated to adjust the disparity of the elderly enrollment, i.e., the insurers with less than national average elderly enrollment will have to contribute more than they are otherwise responsible, while the insurers with higher than national average elderly enrollment will contribute less than they are otherwise responsible. It is still noteworthy that although the EHS ameliorate the financial plight of the municipal National Health Insurance system, it eventually proved to be only a patchwork remedy without a total unification of health insurance system leading to the radical reform in the field of long term care as a form of the Long Term Care Insurance system which effectively unifies the insurers to municipal governments. (3) Preventive Medical Activity component of the EHS Although the EHS was proposed as a patchwork for financial redistribution of the elderly health care cost among different health insurers, another important component was added to the system: publicly funded preventive medical activities starting from the age 40. The preventive medical activities proved to be a major boon for public health field in Japan because ample public fund started to be poured into this field. Mass health screening program for cardiovascular diseases and cancer was much enhanced under these initiatives. Cancer screening was targeted to stomach, uterine, lung, breasts and colon cancers. Many policy debates have been provoked as to the cost-effectiveness of which cancer should be included in the mass screening. However a major and crucial drawback remained between the health care component and preventive medical component of the EHS. They are totally administered as separate entities, the most typical of which are their financing mechanism: the preventive medical activity component is funded by general revenue while the health care component is funded chiefly by contribution from heath insurers premium revenue. Even matching individual health records of mass screening with insurance claims submitted to the NHI division of the municipal governments is seldom, if ever, performed. Because of this separation, the financial reward from preventive medical activities is hard to be felt in health care component operation, both of which are administered in the same municipal government. (4) Action Plans for Long Term Care in Municipal Level To cater to the growing need for long-term care, the hitherto separate policies involving the Elderly Health System and the Elderly Welfare System needed to be effectively integrated at municipal level. In 1990, both laws were amended to require all municipal governments to develop comprehensive action plans based on objective need assessment and service levels to be achieved. Under this initiative, all municipal governments conducted need assessment for long term care in community setting in and around 1993. This survey was unprecedented in that it had covered the entire population of disabled elderly dwelling in home settings and served as a base line for the later development of the Long Term Care Insurance system. |
| 3. Mental Health |
|
Japan's mental health is notoriously characterized by its heavy reliance on hospitalization: the highest per capita psychiatric hospital beds in the world (approximately 360,000 beds), the average length of stay for psychiatric hospitals is 385 days in 1998, and the number of psychiatric patients in hospitals accounts for approximately 0.26 % of the entire population. This "institutionalism" may be partially explained by a historical accident in late 60s in which then U.S. ambassador had been stabbed by a psychiatric patient. This accident provoked a public outcry against danger caused by letting potentially dangerous psychiatric patients in community and called for construction of psychiatric hospital beds to segregate the psychiatric patients from the rest of the society. Then the generally perceived "safety" of Japan's society might partially be made possible at the sacrifice of psychiatric patients' right. On the other hand, a series of scandals involving abuse in some psychiatric hospitals prompted arguments over potential violation of human rights of psychiatric patients. In 1987, the Mental Health Act was amended to assure more emphasis on human right protection of psychiatric patients by tightening the conditions of involuntary hospitalization. Under the Mental Health Act, five forms of hospitalization are stipulated as involuntary hospitalization: detention hospitalization, emergency detention hospitalization, custodial hospitalization, immediate therapeutic hospitalization and observational hospitalization. The most restrictive, detention hospitalization will be granted if the psychiatric patient presents "clear and present" danger to self and/or public as agreed by more than one qualified psychiatrist. Emergency detention hospitalization will be granted for up to 72 hours on the same condition with detention hospitalization with the diagnosis by only one qualified psychiatrist. Custodial hospitalization may be ordered by an attending psychiatrist if the legal custodians agreed without consent of the patient. Immediate therapeutic hospitalization may be ordered by an attending psychiatrist for prompt treatment of the disease. Observational hospitalization will be granted for temporary observation to allow time for the psychiatrist to make diagnoses. Detention hospitalization accounted for nearly 77,000 patients in 1970 but declined sharply ever since. Currently nearly 70% of psychiatric inpatients are voluntary and custodial hospitalization 27.5%. Detention hospitalization accounts for only 1%. |
| 4. Infectious Diseases |
Japan used to be plagues with epidemics of infectious disease, which also claimed a high mortality. The number of reported cases of major traditional infectious disease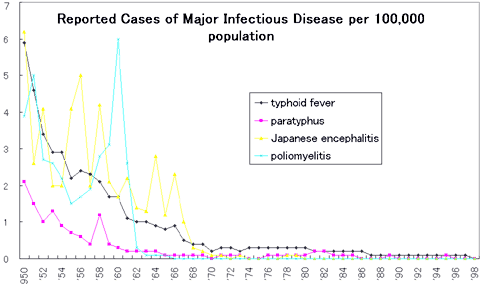 has declined drastically since late 1960s, but so-called emerging and reemerging infectious diseases began to pose renewed public health threats. In 1999, the new Infectious Diseases Control Act was enacted incorporating separate laws against STD, AIDS. Under the new law, infectious diseases are classified into four categories depending on their severity and societal risks. (1) Leprosy Japan used to have the Leprosy Control Act, which was abolished in 1996. The law confined the infected patients to national sanatorium located on isolated islands and continued its practices even after effective treatment became available. Though the law was abolished, it was hard for most patients to return to the society and make their living mainly because majority of them were old. The government now provides public assistance to support those who had been confined to the sanatorium for long time. (2) Viral Hepatitis Viral hepatitis is certainly one of major public health threats in modern Japan. There are estimated to be 1.2 to 1.4 million (more then 1% of population) carriers of HBV and nearly 2 million (1.6% of population) HCV carriers. Hepatitis virus is a known cause of liver cancer. According to a survey, 76% of 30,000 liver cancer deaths in 1997 are attributed to HCV and 17% to HBV. More alarmingly, the number of liver cancer death per population has steadily increased from 14 per 100,000 in 1984 to 24 in 1995 and the increase is solely attributable to HCV. One of the major transmission routes of HCV is iatrogenic. A considerable geographic variance of HCV prevalence might support this hypothesis: some hospitals and clinics used to provide IV treatment without much heed to sterilization and mass immunization programs were occasionally conducted without changing cylinders and needles in the past. Post transfusion hepatitis had been largely eradicated thanks to the introduction of HCV screening introduced in November 1989. Introduction of Interferon to treatment of HBV and HCV to health insurance benefit also contributed to effective treatment of carriers. (3) AIDS 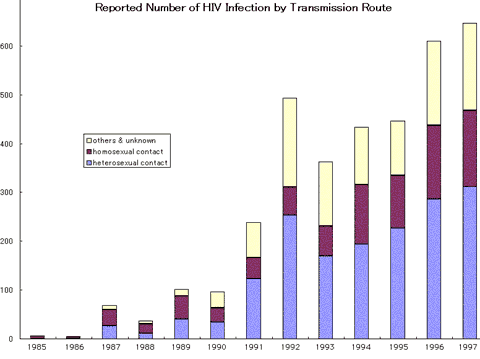 WHO reports that there were 1,987,217 AIDS patients worldwide in 1998. The number of reported HIV positive cases in Japan was 4,347 as of December 1998, of whom 1,316 were non-Japanese. Breakdown by transmission route is: heterosexual transmission 1,400, homosexual transmission 708, blood product 1,434, illicit IV drug use 19, longitudinal infection from mothers 20, others and unknown 766. The cumulative death toll due to AIDS was 1,089 as of December 1998. AIDS epidemic in Japan can be summed up as following six points: The number of reported cases of HIV is constantly growing among Japanese males with transmission routes of home and heterosexual relationship. The number of reported AIDS cases has declined for the first time since the start of surveillance system became fully operational. The number of HIV and AIDS cases involving foreign nationals account for approximately 30% of reported cases in the order of Southeast Asia, Latin America. Sexual intercourse accounts for the largest share of transmission routes and IV drug use and maternal infection account for less than 1%. However, the cases of which transmission routes unknown account for nearly half of the foreign nationals and increasing even among Japanese. Majority of sexual transmission among Japanese took place inside the country for both HIV and AIDS with concentration in and around Tokyo area. However for homosexual intercourse, majority of transmission concentrates in Tokyo. As for geographical distribution, the number of reports from Kinki block (area around Osaka, Kyoto and Kobe) is alarmingly increasing. Although the severity of AIDS epidemic in Japan may be less than other countries in public health perspectives, it draws the regrettable past in which a nearly two thousand of hemophiliac patients had been infected iatrogenically through imported blood product. The dispute over the iatrogenic HIV infection culminated in 1996 when the then health minister officially apologized to the patients and the patients group and the government and pharmaceutical companies had settled according to the recommendation by court. Also in the same year, criminal charges were brought against a leading doctor and a former Ministry of Health officer for professional negligence, but the district court acquitted the doctor in March 2000 ruling that the tragic iatrogenic HIV infection by blood product had not been foreseeable in and around 1985 and therefore the defendant could not be held professionally negligent. (4) Tuberculosis (TB) Japan is still suffering from a high TB mortality in comparison with major developed countries with 2,742 deaths in 1997 or 2.2 per 100,000 population. TB used to be the leading cause of death until as late as 1950 but has dropped to as low as the 22nd rank in 1997. In around 1950, the age specific mortality of TB was highest among young population: nearly 300 per 100,000 population in the 20s making the disease widely quoted in sad stories involving young men and women. Under the TB Control Act, doctors who diagnosed TB patients are required to report to the nearest public health centers to prompt them to keep track of the patient. Public health centers have been serving as the forefront for TB control and prevention. 42,715 new patients were reported in 1997. This translates into 33.9 per 100,000 population. The year 1997 was remarkable because the hitherto declining incidence rate turned upward for the first time in 43 years. Especially the number of active TB patients who are capable of infecting others was 19,213 and did not decline so much since 1975. Once reported, public health centers keep track of the patients until they are diagnosed as free of TB for three years. The cumulative number of patients kept track by public health centers was 121,762 as of December 1997, of whom 55,409 were active TB patients. The TB Control Act require all babies aged 0 to 4 years old to be checked PPD skin test and receive immunization (BCG) for those who showed negative result (no immunity), all of which are publicly funded. If successful, BCG will develop immunity against TB evidenced by positive PPD test. This iatrogenically induced positive PPD test of Japanese citizens is sometimes puzzling to western doctors who naturally interpret the positive skin test as indication of TB infection. In Japan, mildly positive PPD skin test results are interpreted as evidence of immunity developed by BCG vaccination and is usually not interpreted as TB infection if other findings suggest otherwise. Immunity endowed by BCG is not entirely everlasting nor does it provide full protection against TB as evidenced by sporadic outbreaks among young people. The PPD skin test will be repeated in elementary and junior high schools and BCG may be repeated for those students who failed to turn positive and hence no immunity. In 1991, the Pubic Health Committee issued a recommendation with a targeted eradication of TB in the 2030s. In November 1992, the mass chest X-ray exams conducted on all school children in elementary and junior high schools were abolished to reduce unnecessary radioactive exposure, and those with strongly positive PPD skin test were asked to undergo thorough examination at hospitals or clinics. |
| 5. Research and Public Subsidies for Diseases of Scientific Interest |
|
Japan has disease specific research and public subsidies programs for certain diseases. These diseases are called "diseases of scientific interest" and 44 diseases are listed as of 1999. Programs aimed at these diseases consist of two pillars: research grants and public subsidies for patients. Public subsidies for patients will effectively waive the copayment of 20 to 30% of health care cost under the national health insurance system for the treatment related with the diseases on the condition that the patients cooperate with the research programs. |
| 6. Public Assistance for A-Bomb Victim |
|
In recognition of the uniqueness of the A-bomb exposure in Hiroshima and Nagasaki in August 1945, the A-bomb victims are entitled to special public assistance not available for other war casualties. A-bomb victims include those who were exposed intrauterine at the time of bomb blast and those who entered into the bombed area within two weeks. The number of listed victims was approximately 300,000 as of March 1999. The benefit includes public subsidies to waive copayment for health insurance, and cash benefit in the amount of 34,330 yen (approximately 300 dollars) per month for those with chronic diseases not necessarily related to A bomb exposure such as cardiovascular diseases (approximately 80% of those eligible are receiving this cash benefit). As for research activities to study the long-term effect of radiation exposure, a research institute was established under cooperation between Japan and the U.S. in 1975 and its findings are contributing much to the development of radiation exposure standards and protection. |
| 7. Renal Failure |
|
Japan has 79,709 dialysis units and 206,134 dialysis patients as of March 2000, which accounts for roughly one fourth of the world dialysis patients. This reflects a small number of kidney transplantation (only 744 in 2000, of which cadaveric transplantation was only 146) and the generous coverage of health insurance system (for renal dialysis the patients' copayment is capped at 10,000 yen (approximately 80 dollars) per month. Renal failure used to be considered fatal until December 1962, when dialysis was included in health insurance benefit. Still, health insurance subjected the patients to 20 to 30% copayment, which would accumulate to a considerable sum for long-term treatment such as dialysis. In October 1972, public subsidy was introduced to help ease the financial burden of dialysis patients and in October 1984, the Health Insurance Act was amended to cap the monthly copayment for long-term treatment such as dialysis and hemophiliacs to 10,000 yen. 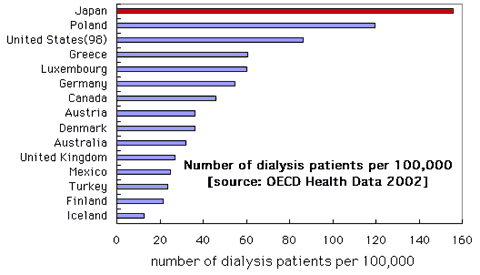 |
| 8. Organ Transplantation |
|
Kidney transplantation was included in health insurance benefit in 1978, but cadaver transplantation was not available in the absence of the law that authorizes removal of organs from corpses. The Cornea and Kidney Transplantation Act was enacted in 1980 to authorize removal of cornea and kidney from corpses on certain conditions, but the dissemination of cadaver transplantation was still hampered by prohibition of organ removal from brain dead bodies. Surgeons had to wait until the heart beat completely stops before they could remove the donated organs, which compromised the success rate of transplantation, although cadaver transplantation was somewhat enhanced by establishing the organ sharing information network in 1983. Also, removal of other organs such as heart, lungs and livers were not yet permitted. Some frustrated patients resorted to traveling abroad to receive transplantations provoking public outcry in some countries and commercial organ transactions in other countries. Even corneal transplantations rely as much as 40% of corneas on import from abroad. In October 1997, the long awaited Organ Transplantation Act was enacted to authorize removal of donated organs from brain dead bodies. As a peculiar twist of legal reasoning, the law authorizes brain death only for those who expressed their wish to donate organs of their choice and consent to acknowledge brain death as their time of death. Moreover the declaration of brain death may only be made after following a strict guideline set forth in the law. Also the law prohibits buying and selling of organs for commercial purposes. In February 1999, the first organ transplant of heart, liver, kidney and cornea removed from a brain dead body was performed under the new law. The number of patients on the waiting list as of March 1999 was, 13,291 for kidney, 17 for heart, 30 for liver and 5 for lungs. As for bone marrow transplant, the bone marrow bank, a database of HLA typing of potential bone marrow donors, was established in December 1991 and maintains a database of over 110,000 potential donors as of May 1999. The bank could successfully match 78% of patients with potential donors and is aiming at 300,000 potential donors to achieve 90% matching rate. |
  
|